An airborne infectious disease isolation room is designed to protect healthcare workers, other patients, and visitors by preventing the spread of airborne pathogens from patients with infectious respiratory illnesses. These patients need to be housed in rooms where the air pressure inside is controlled and maintained at a negative pressure relative to adjacent areas, which minimizes the risk of infectious airborne particles spreading outside the room.
Purpose and Importance
Patients with respiratory infections can transmit pathogens through airborne means, posing a risk of infection to others. An isolation room specifically configured with appropriate airflow and pressure controls helps contain infectious particles and protect others in the facility.
Typical Isolation Room Configuration
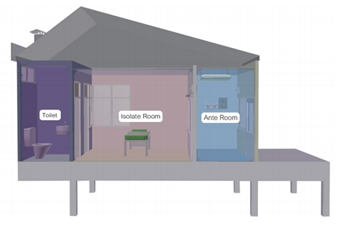
An airborne isolation room is generally organized into three key areas:
- Ante Room (Preparation Area):
A transitional space where healthcare workers prepare before entering the patient room. The ante room typically includes facilities for donning and removing personal protective equipment, and serves as a buffer between the corridor and the patient care area. Its air handling system also helps manage pressure differences between spaces. - Patient Isolation Room:
This is the primary area where the infectious patient is housed. It is equipped with dedicated ventilation systems that continuously circulate and exhaust air to dilute and remove infectious particles near the patient’s breathing zone before discharge from the room. - Toilet/Bathroom for the Patient:
The patient’s bathroom should be accessible directly from the isolation room. It incorporates its own air filtration and ventilation to ensure that air leaving the bathroom meets relevant airflow and pressure control standards.
Airflow and Pressure Control Requirements
To effectively contain airborne pathogens, the isolation room’s HVAC system must maintain a negative pressure differential compared with surrounding areas. This ensures that air flows into the room rather than out of it. The use of HEPA filtration systems within the ventilation helps capture fine airborne particles, reducing the risk of pathogen spread.
Operational Considerations
While isolation rooms are essential for airborne infection control, operational challenges such as patient discomfort, heat, and perceived confinement can affect compliance with their intended use. Ensuring effective pressure control and staff training is crucial to maintaining the performance of the isolation system.
Contextual Notes on HEPA and Pressure Control
For airborne isolation rooms and other controlled environments (e.g., negative-pressure operating rooms), industry practice uses HEPA filters (High-Efficiency Particulate Air filters) that are capable of capturing particles as small as ~0.3 microns at high efficiency. These filters are essential parts of HVAC systems that protect air quality and minimize cross-contamination between spaces.